In recent years, the healthcare industry has seen a massive digital transformation, with mobile apps playing a crucial role in delivering smarter, faster, and more personalized care. As we step into 2026, healthcare app development is entering a new era, powered by advanced technologies, AI-driven solutions, and evolving patient expectations.
Healthcare founders, product managers, CTOs, and digital health entrepreneurs planning to build or upgrade a healthcare app in 2026.
The global mHealth market is projected to surpass $861.40 billion by 2030 — and the companies winning today are those building for the trends of tomorrow. This guide breaks down top healthcare app development trends that are actively reshaping patient care in 2026, with practical insights on how to implement them.
Why Healthcare App Development Has Reached an Inflection Point
The healthcare industry is no longer experimenting with mobile technology — it is depending on it. A decade ago, a hospital app was a patient portal add-on. Today, it is often the primary point of contact between a patient and their care team.
Several forces have converged to make this shift permanent. The COVID-19 pandemic dismantled patient reluctance toward virtual care almost overnight. Post-pandemic, regulators in the US, EU, and across Asia have moved to standardize digital health frameworks. Meanwhile, the economics have shifted too: providers who invested in digital infrastructure during disruption emerged leaner, with better patient retention and lower per-encounter costs.
The result is a market where healthcare app development is no longer optional — it is a strategic imperative. Understanding the key trends shaping this space in 2026 determines whether a digital health product gains adoption or disappears silently.
The Healthcare App Market
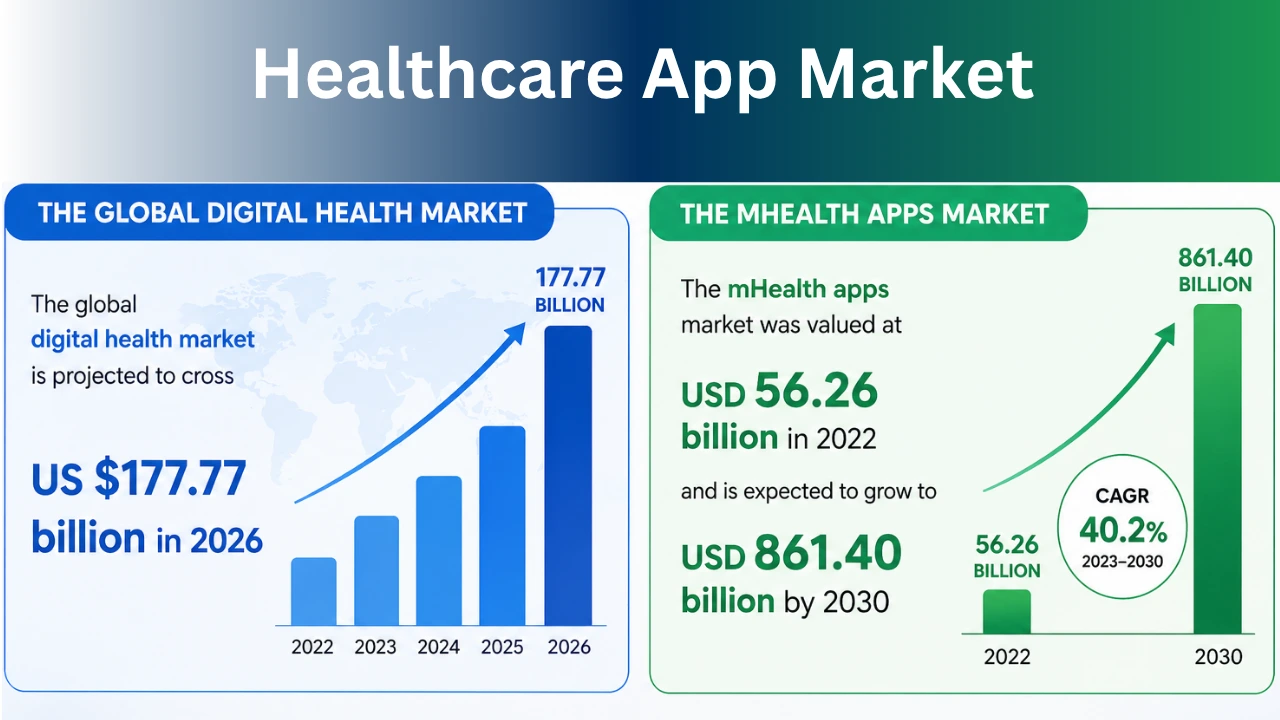
Before diving into trends, ground your strategy in hard data:
- The global digital health market is projected to cross US $177.77 billion in 2026, with mobile healthcare applications contributing a significant share.
- The mHealth apps market was valued at USD 56.26 billion in 2022 and is expected to grow to USD 861.40 billion by 2030, registering a compound annual growth rate (CAGR) of 40.2% over the forecast period.
- More than 78% of patients now prefer mobile-first interactions for non-emergency care.
- Over 65% of new healthcare apps already integrate AI-driven features.
- Around 70% of healthcare providers now offer virtual consultations as a standard service.
- Yet, more than 60% of healthcare apps are abandoned within 30 days — primarily due to poor user experience.
That last data point matters most. It tells us that success in healthcare apps is no longer purely about features or compliance. It is about building meaningful, usable, and intelligent experiences that patients and clinicians actually want to return to.
Types of Healthcare Apps in 2026
Healthcare is not a monolithic domain. Different stakeholders have different needs, and the app categories reflect this diversity:
Patient-Facing Apps
Patient-Facing apps designed to empower individuals symptom checkers, medication reminders, appointment booking, chronic disease trackers, nutrition and fitness logs, and mental wellness tools.
Telehealth Platforms
Telehealth platforms end-to-end virtual care ecosystems offering video consultations, e-prescriptions, remote diagnostics, and AI-powered triage — not just video calls.
Remote Patient Monitoring (RPM) Apps
Remote Patient Monitoring (RPM) apps Connected to wearables and IoT sensors, streaming real-time vitals (heart rate, blood glucose, oxygen saturation) to care teams for proactive intervention.
EHR / EMR Integration Apps
EHR / EMR Integration apps clinical workflow tools that connect to Electronic Health Record systems, enabling seamless data exchange across hospitals, labs, insurers, and pharmacies.
Mental Health Apps
Mental Health apps Virtual therapy, AI chat support, mindfulness tools, and crisis intervention platforms — one of the fastest-growing categories in digital health.
Hospital Operations and Admin Apps
Hospital Operations and Admin apps bed management dashboards, staff scheduling, billing automation, and resource optimization tools that reduce administrative burden on facilities.
Digital Therapeutics (DTx)
Digital Therapeutics (DTx) Software-based, clinically validated treatments for conditions such as diabetes, addiction, ADHD, and depression — increasingly reimbursed by insurers.
Top Healthcare App Development Trends in 2026
1. Artificial Intelligence and Machine Learning at the Core
AI has graduated from pilot projects to production-grade deployment. In 2026, AI is not a differentiator — it is a baseline expectation in modern healthcare app development.
Concretely, AI is powering:
- Predictive analytics that flag high-risk patients before symptoms escalate
- Clinical decision support that assists physicians with differential diagnoses
- Ambient documentation that transcribes patient-physician conversations and auto-generates clinical notes, buying back thousands of clinical hours annually
- AI chatbots providing 24/7 patient triage, post-discharge follow-up, and medication guidance
- Personalized treatment plans derived from analyzing genomic, environmental, and behavioral data simultaneously
Healthcare organizations that automate documentation with ambient AI report immediate operational benefits: clinicians handle higher patient volumes without added headcount, and physician burnout decreases measurably.
Ready to Build Your Healthcare App
Tell us your idea — we’ll give you a free project estimate within 48 hours.
Get a Free Project Estimate →
2. Remote Patient Monitoring (RPM)
Remote Patient Monitoring has crossed from pilot to standard-of-care. In cardiology, diabetes, respiratory care, post-surgical recovery, and elderly care, RPM is now a baseline expectation.
The clinical case is compelling: RPM apps reduce hospital readmissions by nearly 38% and improve medication adherence by over 30%.
The financial case is equally strong. Updated 2026 CMS CPT codes allow providers to generate between $100 and $150 in new monthly reimbursement per enrolled patient through RPM programs, with typical break-even periods of just 2 to 3 months.
Modern RPM apps focus on:
- Real-time dashboards for care team visibility
- AI-driven alerts that distinguish clinically significant changes from noise
- Seamless clinician notifications that integrate with existing EHR workflows
Patient-friendly interfaces that non-technical patients — including elderly populations — can operate independently
3. Telehealth 2.0 — Beyond Video Calls
Telehealth has matured. The version that emerged during the pandemic — essentially a video call bolted onto a scheduling system — has given way to something far more sophisticated.
In 2026, telehealth apps function as complete digital care platforms. They integrate appointment scheduling, virtual waiting rooms, e-prescriptions, remote diagnostics through connected wearables, care plan management, and follow-up automation — all within a single patient journey.
Healthcare app development trends in this space emphasize continuity of care across the entire episode, not one-time virtual visits. Patients expect the same care coordination they receive in person, just accessible from anywhere.
4. Wearables and IoT Integration
Fitness bands and smartwatches have become medical-grade monitoring tools. In 2026, mobile apps are turning consumer wearables into powerful clinical data sources:
- Continuous glucose monitors (CGMs) for diabetic patients
- Smartwatches with FDA-cleared heart rate variability, atrial fibrillation detection, and blood oxygen monitoring
- Biosensors tracking temperature and respiratory rates in real-time
- Implantable devices streaming cardiac data to remote specialists
The transition to 5G technology has been a key enabler, reducing network latency by up to 80% compared to 4G networks. This makes real-time IoT data streaming at clinical fidelity practically feasible at scale.
5. Mental Health and Behavioral Apps
Mental health is among the fastest-growing segments in digital health. The demand is structural: global mental health workforce shortages make it impossible to meet patient demand through traditional in-person therapy alone.
Apps in this category now offer:
- Virtual therapy sessions with licensed therapists, available on-demand
- AI-powered conversational support for anxiety, depression, and crisis intervention
- Mindfulness and stress regulation tools with biometric feedback from wearables
- Mood and behavioral tracking that informs clinician assessments
- Crisis escalation pathways that connect users to emergency services when risk is detected
Regulatory watch: the FDA is increasing scrutiny of mental health apps that make clinical claims. Teams should understand whether their app qualifies as a medical device under SaMD guidance before launch.
6. Interoperability and FHIR Standards
One of the most defining trends in 2026 is mandatory interoperability. Healthcare apps must exchange data seamlessly with hospitals, labs, pharmacies, insurers, and national health systems.
The lack of interoperability costs healthcare systems billions annually through duplicate tests, delayed care decisions, and administrative rework. In the US alone, standardized electronic data exchange has been shown to avoid hundreds of billions in administrative costs annually.
The standards backbone:
- HL7 FHIR (Fast Healthcare Interoperability Resources): RESTful APIs for standardized health data exchange — now the dominant integration standard
- SMART on FHIR: Secure authorization framework enabling third-party apps to access EHR data with patient consent
- TEFCA (Trusted Exchange Framework and Common Agreement): The US government’s national interoperability framework, expanding in 2025–2027
For development teams, this means: interoperability is not a feature you add at the end. It must be architected from the first system design session.
7. Cybersecurity and Privacy-by-Design
Healthcare cybersecurity threats have increased by over 45% year over year. Healthcare data — carrying a black-market value estimated at ten times that of financial records — remains the most targeted dataset in digital security.
In 2026, the industry has shifted to a privacy-by-design model. Security is no longer implemented as a post-development layer; it is embedded from the first line of code.
Mandatory baseline security architecture includes:
- End-to-end encryption for data in transit and at rest
- Role-based access controls (RBAC) limiting data access by job function
- Multi-factor authentication for all clinician-facing portals
- Audit logging tracking every access and modification to Protected Health Information (PHI)
- Regular penetration testing and third-party security audits
- Business Associate Agreements (BAAs) with every third-party vendor handling PHI
Teams that fail to prioritize security are facing not just regulatory penalties — a single HIPAA violation can now reach $2.1 million per violation category — but permanent loss of patient and institutional trust.
8. Blockchain for Healthcare Data Integrity
Blockchain is moving from proof-of-concept to targeted production use in healthcare. It is particularly valuable in scenarios where immutability, transparency, and decentralized access control are required.
High-impact use cases in 2026:
- Patient consent management via smart contracts, giving patients verifiable control over who accesses their records
- Drug supply chain integrity, tracking pharmaceuticals from manufacturer to patient to prevent counterfeiting
- Clinical trial data management, creating tamper-evident audit trails that regulators and sponsors can verify independently
- Credentialing and provider verification, eliminating manual background checks for clinicians moving between systems
The HL7 FHIR standard and blockchain implementations are increasingly combined: FHIR handles standardized data exchange while blockchain ensures data integrity and access control. Research published in peer-reviewed journals confirms that permissioned blockchain architectures — using platforms like Hyperledger Fabric — can meet HIPAA and GDPR compliance requirements when implemented correctly.
Want to integrate Blockchain into your Healhtcare App
Contact Now
9. 5G-Enabled Real-Time Healthcare
5G is not merely faster connectivity for patients streaming video. For healthcare applications, it is infrastructure that makes previously impossible use cases viable:
- Real-time telesurgery and remote procedures with sub-millisecond latency
- Continuous high-fidelity biometric streaming from multiple wearables simultaneously
- Instant large-format medical imaging transfer (MRI, CT) between facilities without compression artifacts
- Augmented reality surgical guidance streamed to headsets in operating theaters
Average 5G speeds of 1–10 Gbps with latency reductions of up to 80% compared to 4G fundamentally change what real-time healthcare interactions can look like.
10. Voice Interfaces and Conversational AI
Typing is no longer the primary interaction method in leading healthcare apps. Voice interfaces are solving two persistent problems: clinical documentation burden and accessibility for elderly or mobility-impaired users.
Applications include:
- Ambient clinical documentation: Physicians speak naturally with patients while the app transcribes, structures, and populates EHR fields automatically
- Voice-activated patient navigation: Patients book appointments, check results, and request prescription refills via spoken commands
- Medication adherence reminders delivered conversationally, with the ability to respond by voice
- Accessibility-first design for patients with visual impairments or limited motor control
Natural Language Processing (NLP) capabilities in 2026 are sophisticated enough to distinguish clinical terminology, handle interruptions, and accurately record medication names with high precision.
11. Personalization and Adaptive UX
One-size-fits-all healthcare apps are rapidly losing market relevance. Studies indicate that personalized healthcare apps improve engagement by over 45% compared to generic alternatives.
Modern healthcare apps adapt in real time based on:
- Health history and chronic conditions surfacing relevant content and alerts
- Behavioral patterns learning when users check in, and optimizing notification timing accordingly
- Wearable data adjusting recommendations based on sleep, activity, and stress signals
- Clinician-defined care plans ensuring patient-facing content aligns with what the care team has prescribed
Over 60% of healthcare apps are uninstalled within the first 30 days. Poor, generic UX is the leading cause. Development teams that invest in adaptive, accessible design see measurably better adoption rates and long-term retention.
12. Digital Therapeutics (DTx)
Digital Therapeutics are software-based interventions that deliver evidence-based therapeutic outcomes for specific medical conditions. They are validated through clinical trials and subject to regulatory oversight — placing them in a category distinct from wellness apps.
The DTx market is expected to reach USD 10.09 billion by 2029, growing at a 10.21% CAGR. Insurance reimbursement for approved DTx products is expanding, creating a viable business model for clinically validated digital health products.
Conditions currently addressed by FDA-authorized DTx include:
- Substance use disorder (reSET-O)
- Insomnia (Somryst)
- ADHD (EndeavorRx)
- Diabetes management programs
Building a DTx product requires clinical trial evidence, regulatory submission (typically De Novo or 510(k) pathway in the US), and a post-market surveillance plan — a significantly longer and more expensive process than standard app development.
13. AR & VR in Healthcare Apps
Augmented and Virtual Reality have found genuine clinical utility in healthcare — moving well beyond novelty into documented patient outcomes improvement. The VR in healthcare market is projected to reach $46.37 billion by 2032 (Fortune Business Insights), with the most validated use cases including surgical training, phobia treatment, chronic pain management, and patient education.
In 2026, AR is active in operating theaters worldwide, overlaying real-time navigation guidance onto a surgical field using HoloLens and similar headsets. VR therapy is FDA-recognized for chronic lower back pain (AppliedVR’s EaseVRx), PTSD treatment, and pediatric procedural anxiety — with some health insurers beginning to reimburse VR therapy sessions. Patient-facing healthcare apps are using AR to give users 3D anatomical explanations of their diagnoses, making complex medical information genuinely comprehensible for the first time.
What to build: For patient-facing apps, AR anatomy visualization (using ARKit on iOS or ARCore on Android) is accessible and high-impact. For B2B clinical apps, VR surgical training modules require Unity or Unreal Engine development with haptic feedback hardware integration — a more substantial investment with a clear ROI in medical education markets.
HIPAA, GDPR, and Regulatory Compliance: What Builders Must Know
Compliance is not a feature. It is a non-negotiable architectural foundation. Here is what matters in 2026:
In the United States:
- HIPAA / HITECH: Governs all apps handling Protected Health Information (PHI). Requires encryption, access controls, audit logging, and Business Associate Agreements with every third-party vendor touching PHI. A single violation category can now result in penalties up to $2.1 million.
- 21st Century Cures Act: Mandates information blocking prohibitions and requires covered entities to support SMART on FHIR APIs for patient data access.
- FDA SaMD Guidance: Applies to AI and software that functions as a medical device — making clinical decisions, diagnosing conditions, or suggesting treatments.
- 42 CFR Part 2: Governs mental health and substance use disorder records, with stricter disclosure rules than standard HIPAA.
Internationally:
- GDPR (EU): Requires explicit patient consent for data processing, right to erasure, data portability, and breach notification within 72 hours.
- Regional regulations in Canada (PIPEDA), Australia (My Health Records Act), and India (DPDP Act 2023) each impose additional requirements for apps serving those markets.
Practical implications for development budgets: Compliance work typically represents 10–15% of total development cost. This is not optional overhead — it is the baseline cost of operating legally in healthcare.
Healthcare App Development Cost Breakdown (2026)
Healthcare app development costs significantly more than consumer apps for three structural reasons: regulatory compliance, integration complexity (EHR systems use specialized data standards), and security requirements.
Cost Ranges by Complexity:
|
App Type |
Complexity |
Estimated Cost Range |
Timeline |
|---|---|---|---|
|
Basic Patient Portal / Appointment App |
Simple MVP |
$50,000 – $100,000 |
8–16 weeks |
|
Telehealth Platform (2 platforms, 1–2 integrations) |
Moderate |
$120,000 – $220,000 |
12–24 weeks |
|
EHR-Integrated Clinical Platform |
Advanced |
$220,000 – $450,000+ |
20–40 weeks |
|
Full-Scale Enterprise Health System |
Enterprise |
$450,000 – $1M+ |
12–24 months |
Key Cost Drivers:
- Compliance architecture: HIPAA/GDPR compliance adds 10–15% to total budget
- EHR integration: Read-only FHIR integrations are relatively affordable; EHR write-back integrations significantly increase cost and timeline
- Platform coverage: iOS + Android + web adds 40–60% over single-platform development; cross-platform frameworks (React Native, Flutter) reduce this gap
- Developer location: US-based teams run $150–$250/hour; offshore teams $30–$80/hour; managed offshore partners offer 40–60% savings while maintaining compliance standards
- Hidden costs: Cloud hosting (AWS/Azure/GCP) adds 10–15% of annual budget; compliance audits add 15–20% on top of build costs; ongoing maintenance typically runs 15–20% of development cost per year
Key Technologies Powering Modern Healthcare Apps
A well-architected healthcare app in 2026 integrates several technology layers:
- Integration Standards: HL7 FHIR, SMART on FHIR, HL7v2, CDA (for legacy system adapters)
- Cloud Infrastructure: AWS (HealthLake, Comprehend Medical), Google Cloud Healthcare API, Microsoft Azure Health Data Services — all offer HIPAA-eligible services under Business Associate Agreements
- AI/ML Frameworks: TensorFlow, PyTorch for model development; pre-trained biomedical NLP models (BioBERT, Med-PaLM) for clinical language understanding
- Wearable Integration: Apple HealthKit (iOS), Google Health API (Android), Bluetooth Low Energy (BLE) protocols for medical device connectivity
- Security: AES-256 encryption, OAuth 2.0 / SMART on FHIR for authorization, SOC 2 Type II certified infrastructure
- Blockchain (where applicable): Hyperledger Fabric for permissioned healthcare networks; Ethereum smart contracts for consent management
How to Choose a Healthcare App Development Partner
A healthcare app development company is different from a standard software agency. When evaluating vendors, look for:
Non-negotiable criteria:
- Demonstrated HIPAA compliance track record (ask for a signed BAA before sharing any PHI)
- Experience with HL7 FHIR and EHR integration (ask for portfolio examples with specific EHR systems)
- HITRUST CSF or SOC 2 Type II certification for their own infrastructure
- Clinical advisory input in their design process — not just engineers making medical UX decisions
Questions to ask:
- Can you show us a Business Associate Agreement workflow for every third-party service that would touch our patient data?
- What is your process for handling regulatory changes mid-project (e.g., a new CMS rule or FDA guidance update)?
- How do you handle EHR vendor change windows and certification queue delays in your project timelines?
- What is your post-launch support and compliance audit process?
Red flags:
- No signed BAA before project start
- Compliance presented as a checkbox, not an architecture decision
- No experience with the specific EHR system you need to integrate with
- Fixed-price contracts for complex EHR integration work (a sign they do not understand the complexity)
Conclusion
Healthcare app development in 2026 is defined by a convergence of forces: AI moving from novelty to infrastructure, interoperability becoming non-negotiable, regulatory frameworks catching up to digital health reality, and patient expectations rising to match consumer technology standards.
The organizations winning in this space are not necessarily those with the largest technology budgets. They are those that understand clinical workflows deeply, treat compliance as architecture rather than paperwork, and obsess over the experience of real users — elderly patients, time-constrained nurses, and overwhelmed physicians — rather than ideal personas.
The opportunity is enormous. The barriers to poor execution are also higher than they have ever been. Build with expertise, build with compliance at the core, and build for the humans whose health depends on getting it right.
At Comfygen, we’ve built healthcare apps across telemedicine, pharmacy, clinical management, health tracking, and laboratory management. We understand the regulatory constraints, the technical complexity, and the human stakes. If you’re planning a healthcare app in 2026, we’d welcome the conversation.
Contact Now:-
Email: sales@comfygen.com
WhatsApp No.: +91-9587867258
FAQs
What is the minimum cost to develop a HIPAA-compliant healthcare app?
HIPAA-compliant MVP — covering basic appointment booking, user registration, and secure messaging — typically starts at $50,000–$80,000. Any app involving EHR integration, AI features, or real-time monitoring will exceed $100,000. Budget for compliance architecture, not just features.
How long does healthcare app development take?
Simple apps take 3–6 months. Mid-complexity telehealth or RPM apps take 6–12 months. Enterprise platforms with deep EHR integration take 12–24 months. EHR vendor certification queues and external compliance reviews are common sources of delay.
Do I need FDA clearance for my healthcare app?
It depends on what your app does. Apps that make clinical claims, diagnose conditions, or suggest treatment decisions typically qualify as Software as a Medical Device (SaMD) and require FDA clearance. Pure wellness, administrative, or patient communication apps generally do not. Consult a regulatory attorney before finalizing your product scope.
What is the difference between a telehealth app and a Digital Therapeutic?
A telehealth app connects patients with clinicians remotely. A Digital Therapeutic (DTx) delivers the therapeutic intervention itself — through software — with clinical evidence supporting its efficacy. DTx products require clinical trials and FDA regulatory clearance; telehealth apps generally do not.
Can I build a healthcare app offshore and still be HIPAA compliant?
Yes, provided your offshore development partner signs a HIPAA Business Associate Agreement, follows your security architecture requirements, and undergoes regular security audits. Many organizations successfully use offshore teams in India, Eastern Europe, or Southeast Asia for healthcare app development while maintaining full HIPAA compliance.
What is FHIR and why does it matter?
FHIR (Fast Healthcare Interoperability Resources) is the dominant standard for exchanging healthcare data between systems via RESTful APIs. If your app needs to connect with hospital EHR systems, insurance platforms, or government health data networks, FHIR compliance is mandatory — not optional.

Mr. Saddam Husen, (CTO)
Mr. Saddam Husen, CTO at Comfygen, is a renowned Blockchain expert and IT consultant with extensive experience in blockchain development, crypto wallets, DeFi, ICOs, and smart contracts. Passionate about digital transformation, he helps businesses harness blockchain technology’s potential, driving innovation and enhancing IT infrastructure for global success.